Defibrillators: The Machine That Brings People Back When Seconds Decide Everything
There are moments in medicine where everything slows down — not because people are calm, but because the situation is so fragile that even one missed second can change a life forever.
And right in the middle of those moments, there’s one machine that becomes the difference between losing someone and pulling them back: the defibrillator.
Everyone has seen it in movies — the paddles, the shout of “Clear!”, the dramatic jolt. But the real story of defibrillators is far more meaningful than a Hollywood scene. This machine isn’t just about electricity. It’s about timing, rhythm, and the hope that the heart can be convinced to beat again.
Today, we’re going deep into the world of defibrillators — how they work, where they came from, and why they remain one of medicine’s most powerful tools.
1. When the Heart Falls Out of Rhythm: Why Defibrillators Exist
The heart is a simple organ on the surface, but what keeps it running is a delicate electrical system.
When this system goes out of sync, even slightly, the heart’s pumping ability collapses. But there’s one rhythm that is especially deadly — ventricular fibrillation (VF).
In VF, the heart doesn’t beat.
Doesn’t pump.
Doesn’t send blood anywhere.
It just quivers like a bag of worms, completely chaotic.
A person collapses.
They stop breathing.
And the clock starts ticking — 4 minutes before the brain begins to take irreversible damage.
That’s why the defibrillator exists.
It isn’t meant to “restart” the heart like people assume, but to reset it — to wipe out the chaotic rhythm and give the heart a chance to reboot normally.
2. The First Attempt: When Electricity Entered Medicine
Before defibrillators existed, cardiac arrest was practically a guaranteed death sentence.
Then in the late 19th century, scientists discovered something curious:
animals whose hearts had stopped sometimes regained rhythm after receiving an electric shock.
But the real breakthrough came in the 1930s when a physiologist named Dr. Claude Beck decided to try it on humans. Hospitals were skeptical. Electricity felt dangerous, unpredictable, and almost unscientific at that time.
Still, in 1947, Beck attempted the first internal human defibrillation during open-heart surgery.
The patient came back.
The heartbeat stabilized.
And suddenly the impossible wasn’t impossible anymore.
From that single moment, medicine changed direction.
3. External Defibrillators: Shock From the Outside
Internal shocks worked — but they were only possible during open surgery.
Doctors needed something that worked on a collapsed patient in an emergency room, in the street, in an ambulance.
Soon came the first external defibrillators. They were huge, heavy, and required a solid understanding of physiology. Nurses had to apply conductive gel, handle metal paddles, and set the correct voltage.
They were powerful, messy, and honestly a little terrifying — but they saved lives.
By the 1960s and 70s, ambulances were being equipped with portable versions, turning emergency medicine into the life-saving system it is today.
4. How a Defibrillator Really Works (In Normal Human Words)
A defibrillator doesn’t “jump-start” the heart.
It doesn’t force it to beat.
Here’s the real mechanism:
-
The machine builds a controlled electrical charge.
-
This charge is delivered through electrodes or paddles.
-
The electrical surge depolarizes the entire heart muscle at once.
-
All chaotic electrical activity stops for a split second.
-
The heart’s natural pacemaker takes over and restarts a normal rhythm — if possible.
It’s less like restarting a car and more like rebooting a frozen computer.
The shock isn’t magic.
It simply erases the chaos.
5. Types of Defibrillators: Not All Are the Same
We all know the dramatic ones shown in movies, but there are several types with very different uses.
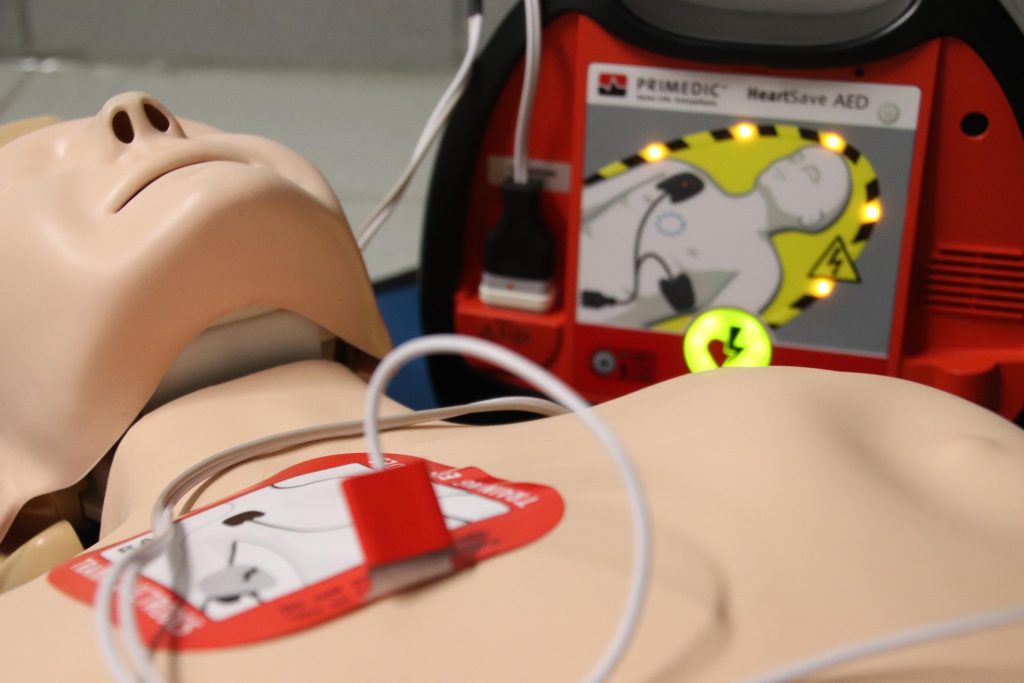
1. AED (Automated External Defibrillator)
These are the small, bright boxes found in airports, malls, gyms, and even schools. They’re designed for regular people — no medical training needed.
You open it.
Follow the voice instructions.
The machine analyzes the heart rhythm on its own.
It decides whether a shock is needed.
AEDs have saved countless lives because they bring treatment close to the victim before medical professionals arrive.
2. Manual Defibrillators
Used by doctors and paramedics.
They require expert judgment to choose:
-
the energy level
-
when to shock
-
which rhythm to shock
These are the paddles you see in hospitals and emergency departments.
3. ICD (Implantable Cardioverter Defibrillator)
A small device implanted inside the chest — like a mini defibrillator living inside the body.
It monitors the heart 24/7 and gives a shock automatically if a dangerous rhythm appears.
For people with severe heart disease, an ICD is like having a guardian inside their chest.
4. Wearable Defibrillators
A vest-like device used temporarily for patients waiting for ICD implantation or recovering from surgery.
6. Inside the Machine: What Makes a Defibrillator Work?
Even though the job sounds simple — “give a shock” — the engineering behind a defibrillator is incredibly precise.
Inside you’ll find:
-
a capacitor (stores the electrical charge)
-
control circuitry
-
ECG system to interpret heart rhythms
-
energy selectors
-
software that analyzes patterns in milliseconds
The goal is to deliver just the right amount of energy — too little does nothing, too much can cause severe damage.
A defibrillator must walk a tightrope between life and injury, and the balance is almost mathematical.
7. Real-Life Impact: Stories That Happen Every Day
The power of this machine isn’t just in theory — it shows up in everyday stories.
A man collapses while jogging in a park.
A teenager faints suddenly in a school gym.
An elderly woman stops breathing at home.
In all these moments, people have seconds to act.
And over and over again, someone grabs an AED, sticks on the pads, follows the machine’s calm voice prompts — and the person comes back.
It’s one of the few medical tools that gives everyday people the power to save a life.
8. Misconceptions About Defibrillators
Here are a few things people get wrong:
“You can shock a flatline back to life.”
No — that only works in movies.
Flatline (asystole) doesn’t respond to defibrillation.
“Defibrillators always work.”
They don’t.
Sometimes the heart is too damaged or too oxygen-deprived.
“Only doctors should touch them.”
AEDs are literally designed for the public.
Their instructions are fool-proof.
“The shock restarts the heart.”
Technically, the shock stops the chaos, not starts the heartbeat.
9. The Future: AI, Smart Monitoring, and Ultra-Portable Devices
Defibrillators are evolving faster than ever.
The newest models can:
-
detect rhythms with incredible accuracy
-
filter background noise
-
provide CPR feedback
-
suggest energy levels
-
connect to emergency control centers
-
send data instantly to hospitals
Researchers are now working on:
-
ultra-miniature implantable devices
-
AI that predicts cardiac arrest before it happens
-
shock-free defibrillation using targeted ultrasound
The future may not rely on electricity at all — some early prototypes use focused pulses to reset rhythm without the dramatic shock.
Imagine a world where a patient never collapses because their device warns them minutes in advance.
That’s the direction we’re heading.
10. Final Thoughts: A Device That Holds Life in Its Hands
Of all the medical instruments ever created, the defibrillator stands in a category of its own.
It doesn’t diagnose.
It doesn’t monitor.
It doesn’t prevent.
It rescues.
Pure and simple.
It’s the tool that steps in when everything else fails.
It’s the last line of defense when the heart gives up.
And every person saved by it carries a quiet reminder that sometimes, technology isn’t cold or distant — sometimes it’s the only reason someone gets a second chance.